You know what they say: Life is full of unexpected twists and turns. And if you belong to the 23 percent of U.S. adults with varicose veins, there’s a good chance that so are your limbs.
“Varicose veins are swollen, twisted, and enlarged veins that can occur anywhere in the body but are most commonly found in the legs,” explains David Seitz, M.D., a board-certified doctor from New York. “They can be blue, purple, or skin-colored and appear as bulging, ropey cords just beneath the surface of the skin.”
Varicose veins form when the valves inside the veins become weak or damaged – that is, they lose their elasticity. Normally, these valves open and close to keep your blood flowing in one direction – but when they weaken, Seitz says, “The blood can lean backward and accumulate in the veins, causing them to swell.”
Are Varicose Veins Serious?
Here’s the good news: in most cases, varicose veins are simply a cosmetic concern – especially when they first appear. Despite being unsightly, these colorful coils are rarely indicative of a serious health condition.
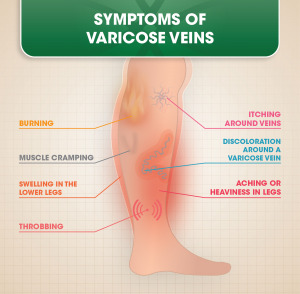
In some cases, however, these swollen veins may become symptomatic. Symptoms of varicose veins can include an achy or heavy feeling in the legs, swollen ankles and feet, muscle cramps, itching around the veins, and pain that increases after sitting or standing. When varicose veins cause discomfort, it may be time to consider treatment. (We’ll get to that in a minute.)
Who Is At Risk For Developing Varicose Veins?
Now for some bad news: varicose veins are largely hereditary. In fact, if you have one parent who has varicose veins, your chance of developing them increases by 40 percent. And if both of your parents have them, your risk skyrockets to 90 percent.
Another risk factor you can’t control is (you guessed it) female sex. While both men and women can develop varicose veins, women are nearly twice as likely to have them, thanks to the valve-weakening effects of estrogen and progesterone. (These are the same female hormones responsible for your pesky period symptoms, by the way).
Other factors that increase your risk of developing varicose veins include aging, pregnancy, obesity, or prolonged sitting or standing, Seitz explains. A history of leg trauma, too, can place you at a greater risk because injury can damage the valves inside the veins.
Prevention/ Varicose Veins Treatment
Back to the good news: While you can’t completely prevent varicose veins from forming, you can decrease your risk of developing them by making certain lifestyle changes. And if you’re already grappling with the bulging twists and turns, these practical steps can help relieve discomfort or stop your condition from getting worse.
Here are four lifestyle changes you can adopt right now to prevent or treat varicose veins, says Seitz:
-
Exercise regularly. “Exercise helps to improve circulation throughout your body and can help reduce the chances of developing varicose veins,” Seitz explains. Aim for 30 minutes of moderate exercise (like walking) at least five days a week.
-
Wear compression stockings. Compression stockings are tight-fitting socks that squeeze your legs and help increase blood flow from your legs to your heart. “This helps to reduce the pressure on your veins and can help prevent varicose veins from forming,” Seitz says.
Hi Clasmix Knee-High Compression Socks
-
Elevate your legs. “Elevating your legs can help relieve the pressure on your veins and improve circulation,” Seitz points out. “Try to take breaks throughout the day, and try to raise your legs above the level of your heart when you can,” he recommends.
-
Maintain a healthy weight. “Being overweight or obese increases your risk of developing varicose veins, so maintaining a healthy weight is important for prevention,” Seitz explains. Eating a balanced diet and exercising regularly can help you maintain a healthy weight.
When Should I See A Medical Professional?
If lifestyle changes aren’t enough to prevent or treat varicose veins, Seitz points out, medical treatment may be necessary. The good news (again) is that these treatments tend to be minimally invasive, including laser therapy and sclerotherapy.
“Laser therapy uses lasers to heat the vein walls and cause them to collapse, while sclerotherapy involves injecting a solution into the veins that causes them to harden and eventually fade away,” Seitz explains. “Surgery may also be an option for more severe cases, where the veins are removed entirely.”
Aching to banish the bulge in your legs once and for all? Contact your primary care provider, who may refer you to a dermatologist, vein specialist, or vascular surgeon, depending on the treatment you need. In most cases, if your varicose veins are causing discomfort, your health insurance will help cover the cost.

Have you struggled with varicose veins? What helped to relieve your symptoms? Share your recommendations in the comments!
Keep Scrolling To Read More Health And Wellness Articles: